Assisting an unwell infant in achieving restful slumber is a multifaceted endeavor, demanding attention to the specific symptoms presented and employing various supportive strategies. The core objective involves mitigating discomfort and establishing a conducive sleep environment for the child. For instance, addressing nasal congestion through gentle saline drops and bulb syringe aspiration can significantly improve breathing and consequently, sleep quality.
Prioritizing the sleep of an ailing baby offers substantial advantages. Adequate rest bolsters the infant’s immune system, facilitating recovery and minimizing the duration of the illness. Furthermore, consistent sleep patterns, even during sickness, contribute to the baby’s overall well-being and emotional regulation. Historically, caregivers have recognized the crucial role of sleep in convalescence, often employing remedies and techniques passed down through generations to soothe and comfort sick infants.
Subsequent sections will delve into specific methods for promoting sleep in sick babies. These include modifying the sleep environment, administering appropriate medications or remedies (as directed by a healthcare professional), employing comforting techniques, and adjusting feeding schedules to accommodate the infant’s needs during illness.
Guidance for Facilitating Sleep in Sick Infants
The following recommendations aim to provide caregivers with practical approaches to improve sleep quality for infants experiencing illness. These suggestions emphasize creating a comfortable and supportive environment to promote rest and recovery.
Tip 1: Maintain Hydration: Adequate fluid intake is crucial. Offer frequent, small amounts of breast milk or formula to prevent dehydration, which can exacerbate discomfort and disrupt sleep.
Tip 2: Clear Nasal Passages: Nasal congestion significantly impairs breathing. Use saline drops followed by gentle suction with a bulb syringe to clear the nasal passages before bedtime and as needed throughout the night.
Tip 3: Elevate the Head: Slightly elevate the infant’s head during sleep. This can be achieved by placing a towel or small blanket under the mattress (never directly under the baby) to help drain nasal passages and ease breathing. This should be done carefully and only if safe.
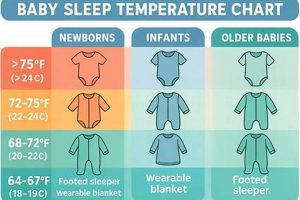
Tip 4: Regulate Room Temperature: Ensure the room is comfortably cool and well-ventilated. Overheating can be detrimental, while excessive cold may cause shivering and discomfort.
Tip 5: Employ White Noise: Consistent background noise, such as a fan or white noise machine, can mask disruptive sounds and promote a calming sleep environment.
Tip 6: Provide Comfort Measures: Gentle rocking, swaddling (if age-appropriate and safe), and quiet singing can provide reassurance and promote relaxation.
Tip 7: Monitor Symptoms: Closely observe the infant for any worsening symptoms or new developments that require immediate medical attention. Accurate monitoring allows for timely intervention and prevents sleep disruption due to escalating discomfort.
Tip 8: Consult Healthcare Professionals: Seek advice from a pediatrician regarding appropriate medications or remedies to alleviate specific symptoms contributing to sleep disturbances. Adhering to professional guidance ensures safe and effective treatment.
Implementing these strategies can significantly improve the likelihood of a restful night for a sick infant, contributing to a faster recovery and improved overall well-being. Creating a nurturing and comfortable sleep environment is paramount during illness.
The following section will address potential challenges and complications associated with managing infant sleep during periods of sickness, along with guidance on when to seek professional medical assistance.
1. Comfort
The provision of comfort is a fundamental aspect of facilitating sleep in sick infants. Discomfort stemming from illness, whether caused by fever, congestion, or pain, directly inhibits the ability to fall asleep and maintain restful slumber. Consequently, addressing the sources of discomfort becomes paramount in the pursuit of improved sleep. For example, a feverish infant may experience chills and restlessness; therefore, adjusting room temperature and providing lightweight, breathable clothing can mitigate these sensations and foster a more conducive sleep environment. Similarly, an infant experiencing nasal congestion may find it difficult to breathe while lying down; elevating the head of the crib and using a humidifier can alleviate respiratory distress and promote easier breathing during sleep.
The importance of comfort extends beyond addressing physical symptoms. Emotional comfort, provided through parental presence and soothing techniques, plays a vital role in calming an anxious or distressed infant. Gentle rocking, humming, or singing familiar lullabies can create a sense of security and promote relaxation, making it easier for the infant to drift off to sleep. A tangible illustration lies in the practice of swaddling newborns; this technique provides a sense of containment and security that mimics the womb, effectively reducing startle reflexes and promoting longer, more restful sleep. The integration of tactile comfort with targeted symptom relief can create a synergistic effect, maximizing the potential for achieving restorative rest.
In conclusion, the pursuit of sleep for sick infants necessitates a holistic approach that prioritizes comfort in both its physical and emotional dimensions. By identifying and mitigating sources of discomfort, caregivers can create a more favorable environment for sleep, ultimately supporting the infant’s recovery and overall well-being. While addressing symptoms and providing physical comfort are crucial, the significance of emotional reassurance should not be underestimated. These combined efforts are essential to help sick babies sleep.
2. Hydration
Adequate hydration is a critical factor influencing an infant’s sleep, particularly when the infant is experiencing illness. Dehydration can exacerbate discomfort, leading to restlessness and sleep disruption. Ensuring sufficient fluid intake is, therefore, a key component in facilitating rest for sick babies.
- Thickened Secretions and Nasal Congestion
Dehydration thickens mucus secretions, intensifying nasal congestion. Increased congestion makes breathing more difficult, especially when lying down. Clearer airways promote easier breathing and, consequently, improved sleep. Maintaining hydration helps thin these secretions, facilitating easier removal and reducing respiratory distress.
- Fever Management and Thermoregulation
Fever, a common symptom of illness, can lead to fluid loss through perspiration. Dehydration resulting from fever impairs the body’s ability to regulate temperature effectively. Replenishing fluids assists in temperature regulation, reducing discomfort associated with both high and low body temperatures, thus promoting a more stable sleep environment.
- Gastrointestinal Upset and Electrolyte Balance
Illnesses often manifest with gastrointestinal symptoms such as vomiting and diarrhea, leading to significant fluid and electrolyte loss. Electrolyte imbalances can cause muscle cramps and irritability, both of which disrupt sleep. Oral rehydration solutions, as directed by a healthcare professional, can restore fluid and electrolyte balance, reducing discomfort and promoting relaxation conducive to sleep.
- Medication Administration and Effectiveness
Dehydration can affect the absorption and efficacy of certain medications. For example, some medications require adequate fluid volume for proper distribution throughout the body. Maintaining hydration ensures that medications, when prescribed by a physician, are administered effectively and can alleviate symptoms contributing to sleep disturbances.
In summary, hydration plays a vital role in several physiological processes that directly impact an infant’s sleep quality during illness. By addressing dehydration, caregivers can mitigate discomfort stemming from congestion, fever, gastrointestinal upset, and ineffective medication administration, leading to more restful sleep and improved recovery.
3. Congestion Relief
Nasal congestion is a primary impediment to infant sleep during periods of illness. An infant’s inability to effectively clear nasal passages leads to labored breathing, discomfort, and frequent awakenings. Thus, effective congestion relief is inextricably linked to improved sleep outcomes for sick babies.
- Saline Nasal Drops and Suctioning
The administration of saline nasal drops followed by gentle suctioning using a bulb syringe serves to loosen and remove mucus from the nasal passages. This intervention directly clears the airway, facilitating easier breathing. For instance, prior to bedtime, instilling a few drops of saline in each nostril and subsequently suctioning the mucus can significantly reduce nighttime congestion and improve sleep duration. This technique addresses the physical obstruction caused by mucus accumulation.
- Humidification
Introducing moisture into the air through the use of a humidifier helps to thin nasal secretions, making them easier to expel. Dry air exacerbates congestion; therefore, a humidifier creates a more conducive environment for respiratory comfort. Running a cool-mist humidifier in the infant’s room, particularly during sleep, can alleviate congestion and promote smoother breathing throughout the night. The increased humidity counteracts the drying effects of indoor heating, which often worsens congestion.
- Elevated Positioning
Slightly elevating the infant’s head during sleep aids in the drainage of nasal passages. Gravity assists in moving mucus away from the upper airway, reducing congestion-related discomfort. This can be achieved by placing a towel or small blanket under the mattress (never directly under the baby). While this method does not actively clear congestion, it facilitates its natural drainage, thus minimizing breathing difficulties during sleep. Caution must be exercised to ensure the incline is moderate and does not compromise infant safety.
- Avoiding Irritants
Exposure to environmental irritants, such as cigarette smoke, strong perfumes, and dust, can exacerbate nasal congestion. Minimizing these irritants in the infant’s environment is essential for preventing further inflammation and mucus production. Maintaining a smoke-free and dust-free home environment can significantly reduce congestion-related sleep disturbances. Eliminating potential triggers prevents the worsening of symptoms and supports respiratory comfort.
The application of these congestion relief strategies directly contributes to the goal of promoting restful sleep in sick infants. By addressing the physiological mechanisms underlying nasal congestion, caregivers can significantly improve the infant’s breathing comfort and, consequently, their ability to achieve restorative sleep. The consistent and appropriate implementation of these techniques forms an integral part of a comprehensive approach to managing infant illness and promoting overall well-being.
4. Temperature regulation
Body temperature regulation plays a pivotal role in facilitating sleep for sick infants. Deviations from the optimal thermal range, whether hypothermia or hyperthermia, induce physiological stress that directly disrupts sleep patterns. An elevated temperature, commonly associated with fever, triggers increased metabolic activity and discomfort, making it difficult for the infant to settle and maintain restful sleep. Conversely, a body temperature that is too low can also disrupt sleep due to shivering and increased energy expenditure to generate heat. Therefore, maintaining a stable and appropriate thermal environment is essential for promoting sleep and supporting the infant’s recovery process.
The practical application of temperature regulation strategies involves several key considerations. Monitoring the infant’s temperature regularly allows for timely interventions. If a fever is present, antipyretic medications, as prescribed by a healthcare professional, can help to lower the temperature and alleviate discomfort. Adjusting the infant’s clothing and bedding to prevent overheating or chilling is crucial. A room temperature that is comfortably cool promotes heat dissipation and prevents excessive sweating, which can further disrupt sleep. Real-life examples include using lightweight, breathable clothing during warmer periods and adding an extra layer of clothing or a thin blanket during colder periods. Caregivers should also be mindful of environmental factors, such as avoiding direct sunlight or drafts that could impact the infant’s temperature.
In conclusion, temperature regulation is an indispensable component of promoting sleep for sick infants. Maintaining a stable and appropriate thermal environment minimizes physiological stress and enhances the infant’s comfort, thereby facilitating restful sleep. Challenges may arise in accurately assessing and managing temperature fluctuations, particularly in infants with underlying medical conditions. However, a diligent approach to monitoring temperature, adjusting the environment, and administering appropriate medications, under professional guidance, can significantly improve sleep outcomes and contribute to the infant’s overall well-being and recovery. Ensuring temperature stability directly impacts the effectiveness of other sleep-promoting strategies, highlighting its fundamental importance.
5. Soothing techniques
Soothing techniques constitute a critical element in facilitating sleep for sick infants. The discomfort and distress associated with illness often manifest as increased irritability and difficulty self-soothing. Consequently, implementing appropriate soothing techniques becomes paramount in calming the infant and creating a conducive environment for sleep. Effective soothing methods address both physical and emotional needs, mitigating the factors that disrupt sleep patterns in sick infants. For example, gentle rocking mimics the motion experienced in the womb, providing a sense of security and reducing anxiety. Similarly, the consistent application of white noise masks disruptive environmental sounds, promoting a calmer and more predictable sleep environment. The selection and application of soothing techniques must be tailored to the individual infant’s temperament and the specific symptoms being experienced.
The practical application of soothing techniques varies based on the nature of the illness and the infant’s individual preferences. For an infant experiencing respiratory distress due to nasal congestion, gentle chest percussion combined with positional changes can aid in mucus mobilization and promote easier breathing. Alternatively, for an infant with gastrointestinal discomfort, a warm compress applied to the abdomen may alleviate cramping and promote relaxation. Furthermore, consistent and predictable bedtime routines that incorporate soothing elements, such as a warm bath, a gentle massage, or a quiet story, can signal to the infant that it is time to sleep, thereby promoting a sense of security and predictability. The effectiveness of soothing techniques is often enhanced when combined with other sleep-promoting strategies, such as maintaining a comfortable room temperature and ensuring adequate hydration. In essence, soother techniques reduce the symptoms that prevent baby sleep well.
In summary, the strategic deployment of soothing techniques is essential for facilitating sleep in sick infants. These techniques address both the physical and emotional dimensions of discomfort, creating a more conducive environment for rest and recovery. Challenges may arise in identifying the most effective soothing methods for individual infants and adapting these techniques as the infant’s condition evolves. However, a consistent and responsive approach to soothing, guided by observation and parental intuition, can significantly improve sleep outcomes and promote the overall well-being of the sick infant. Ultimately, the ability to soothe a distressed infant is invaluable in providing comfort and support during periods of illness, and improving sleep.
6. Medical guidance
Expert medical guidance is a cornerstone of effective care when an infant is unwell. Navigating the complexities of illness requires accurate diagnosis and appropriate interventions, both of which directly influence the quality and duration of sleep.
- Accurate Diagnosis
An accurate diagnosis provides the foundation for targeted treatment. Symptoms such as fever, cough, or irritability may stem from various underlying conditions. A healthcare professional can differentiate between viral infections, bacterial infections, or other medical issues. For example, an undiagnosed ear infection may cause significant discomfort that disrupts sleep. Addressing the underlying cause through appropriate medication, as prescribed by a physician, directly alleviates discomfort and promotes improved sleep. Misdiagnosis or delayed diagnosis can prolong suffering and impede the infant’s ability to rest.
- Medication Management
Pharmacological interventions, when indicated, require careful medical oversight. Dosage, frequency, and potential side effects must be considered to ensure both safety and efficacy. For example, administering the incorrect dosage of a fever-reducing medication can be ineffective or harmful. Certain medications may also have sedative or stimulant effects that impact sleep patterns. A healthcare provider can provide guidance on appropriate medication choices and administration protocols to minimize adverse effects and maximize therapeutic benefits. Responsible medication management ensures that interventions support, rather than disrupt, the infant’s sleep cycle.
- Symptom-Specific Interventions
Medical guidance extends beyond general treatment to encompass symptom-specific interventions tailored to the infant’s unique presentation. For instance, infants with bronchiolitis may benefit from nebulized treatments to open airways, while those with gastroesophageal reflux may require dietary modifications or positional therapy. These interventions alleviate the specific symptoms contributing to sleep disturbances. A healthcare professional can assess the infant’s individual needs and recommend appropriate strategies to mitigate discomfort and promote restorative rest. Individualized symptom management is crucial for optimizing sleep outcomes during illness.
- Red Flags and Emergency Care
Medical guidance provides critical information regarding potential warning signs that necessitate immediate attention. Symptoms such as difficulty breathing, high fever unresponsive to medication, or signs of dehydration require prompt medical evaluation. Recognizing these red flags and seeking timely intervention can prevent serious complications and minimize the impact on the infant’s well-being. Access to reliable medical advice ensures that caregivers are equipped to identify and respond to potentially life-threatening situations, thereby safeguarding the infant’s health and preventing prolonged sleep disturbances due to escalating illness.
The multifaceted nature of medical guidance underscores its importance in promoting sleep in sick infants. Accurate diagnosis, responsible medication management, symptom-specific interventions, and awareness of red flags contribute to a comprehensive approach that prioritizes the infant’s health and well-being. The integration of medical expertise with supportive care strategies optimizes the potential for restorative sleep and facilitates a faster recovery. Ignoring or neglecting medical guidance can have detrimental consequences, highlighting its central role in ensuring the health and safety of sick infants.
7. Symptom monitoring
Diligent observation of an infant’s symptoms is paramount in guiding effective strategies designed to promote sleep during illness. Symptom monitoring informs decisions related to comfort measures, medical interventions, and environmental adjustments, all of which directly impact the infant’s ability to achieve restful sleep. Accurate and timely symptom assessment is essential for tailoring care and optimizing sleep outcomes.
- Fever Tracking and Management
Monitoring the infant’s temperature at regular intervals allows for early detection of fever, a common symptom that significantly disrupts sleep. Accurate temperature readings facilitate informed decisions regarding antipyretic administration and appropriate cooling measures. For example, an increase in temperature beyond a certain threshold may prompt the use of medication to reduce fever-related discomfort, making sleep more attainable. The absence of fever may preclude the use of such medication, preventing unnecessary intervention and minimizing potential side effects that could further disrupt sleep.
- Respiratory Distress Assessment
Observing respiratory rate, effort, and the presence of abnormal sounds such as wheezing or stridor provides critical information regarding the infant’s respiratory status. Increased respiratory effort or signs of airway obstruction necessitate interventions aimed at improving breathing, such as nasal suctioning or positional changes. Recognizing these signs early can prevent episodes of respiratory distress that abruptly awaken the infant. Moreover, changes in respiratory patterns may indicate the need for medical evaluation, leading to timely intervention and preventing more severe sleep disruptions.
- Hydration Status Evaluation
Assessing hydration status through monitoring urine output, skin turgor, and the presence of dry mucous membranes provides insights into the infant’s fluid balance. Dehydration exacerbates discomfort and contributes to restlessness, both of which impair sleep. Recognizing signs of dehydration allows for prompt fluid replacement, either orally or intravenously, depending on the severity. Maintaining adequate hydration mitigates discomfort and promotes a more stable physiological state conducive to sleep. Conversely, overhydration can also disrupt sleep; therefore, balanced assessment is essential.
- Behavioral and Comfort Cue Recognition
Observing the infant’s behavioral cues, such as irritability, fussiness, and the expression of discomfort, provides valuable information regarding their overall well-being. Recognizing these cues allows caregivers to implement targeted comfort measures, such as gentle rocking, swaddling, or offering a pacifier. These interventions address underlying discomfort and promote relaxation, facilitating the onset of sleep. Ignoring these cues can lead to prolonged periods of distress, making it more difficult for the infant to settle and maintain restful sleep. Responsive caregiving, guided by symptom monitoring, is essential for promoting sleep in sick infants.
In conclusion, diligent symptom monitoring forms the bedrock of effective sleep-promoting strategies for sick infants. The insights gained from accurate symptom assessment inform targeted interventions designed to alleviate discomfort, optimize physiological stability, and promote relaxation. Regular observation and responsive caregiving are essential for navigating the challenges of infant illness and maximizing the potential for restorative sleep. Effective sleep promotion requires a comprehensive and responsive approach, with symptom monitoring serving as the guiding principle.
Frequently Asked Questions
This section addresses common inquiries related to improving sleep quality for infants experiencing illness, providing evidence-based guidance and practical recommendations.
Question 1: Is it advisable to let a sick baby sleep longer than usual?
While prolonged sleep can be beneficial, observe the infant for any signs of distress or dehydration. Ensure regular feeding and hydration, even if the infant is sleeping more than normal. Consult with a healthcare provider if there are concerns about lethargy or decreased responsiveness.
Question 2: How can nasal congestion be safely managed to improve sleep?
Employ saline nasal drops followed by gentle suction using a bulb syringe to clear nasal passages before sleep. A cool-mist humidifier can also help to thin mucus secretions, promoting easier breathing. Positional therapy, such as slightly elevating the head of the crib, may facilitate drainage.
Question 3: What measures can be taken if a sick baby refuses to sleep in a crib?
Temporary co-sleeping, adhering to safe sleep guidelines, may provide comfort. However, prioritize transitioning the infant back to the crib as symptoms improve. Consider placing a familiar-smelling item, such as a worn t-shirt, in the crib to provide reassurance.
Question 4: Are over-the-counter medications safe for promoting sleep in sick babies?
Administering any medication, including over-the-counter options, requires consultation with a healthcare professional. Some medications may be contraindicated or may have adverse effects. Adherence to medical advice ensures safe and effective symptom management.
Question 5: What environmental adjustments can optimize sleep for a sick infant?
Maintain a comfortably cool and well-ventilated room. Minimize noise and light exposure. Avoid exposure to environmental irritants, such as smoke or strong fragrances. A consistent bedtime routine can also promote a sense of security and predictability.
Question 6: When should medical intervention be sought for a sick baby struggling to sleep?
Seek medical attention if the infant exhibits difficulty breathing, high fever unresponsive to medication, signs of dehydration, lethargy, or any other concerning symptoms. Prompt medical evaluation can prevent complications and ensure appropriate treatment.
Prioritizing comfort, maintaining hydration, and managing symptoms under medical guidance are crucial. Symptom monitoring plays a vital role in understanding the individual needs.
The subsequent section will address potential challenges and complications associated with managing infant sleep during periods of sickness, along with guidance on when to seek professional medical assistance.
Conclusion
This exposition has detailed the multifaceted strategies required to promote sleep in sick infants. Key considerations include symptom management, environmental modifications, and adherence to medical guidance. The provision of comfort, maintenance of hydration, and relief of congestion are critical components of a comprehensive approach. Understanding these principles is essential for caregivers seeking to optimize sleep outcomes for unwell infants.
Prioritizing the well-being of an ailing infant necessitates a commitment to evidence-based practices and responsive caregiving. Recognizing the significance of sleep in the recovery process underscores the importance of implementing these strategies consistently and diligently. Continued research and refinement of these methods will further enhance the ability to support infant health and promote restorative rest during periods of illness.


![Baby Sleepwear: What Should Baby Wear to Sleep? [Guide] Baby Care 101: Essential Tips for Happy, Healthy Babies Baby Sleepwear: What Should Baby Wear to Sleep? [Guide] | Baby Care 101: Essential Tips for Happy, Healthy Babies](https://singlebabies.com/wp-content/uploads/2026/04/th-491-300x200.jpg)